That is an excerpt from Second Opinion, a weekly evaluation of well being and medical science information emailed to subscribers Saturday mornings. In the event you haven’t subscribed but, you are able to do that by clicking clicking right here.
Emergency rooms throughout Canada are dealing with a rising disaster — staffing shortages, burnout, worsening wait-times, closures, an absence of sufficient funding and a surge of sufferers searching for pressing care, all threatening to overwhelm a system getting ready to collapse.
This isn’t the identical sort of stress they confronted in the course of the COVID-19 pandemic, however medical doctors and nurses throughout the nation who spoke to CBC Information say the present pressure on ERs can really feel worse now than it was in the course of the previous few years.
Dr. Yogi Sehgal, an ER doctor at Dr. Everett Chalmers Regional Hospital in Fredericton, mentioned his emergency division narrowly prevented catastrophe a number of weeks in the past when a number of critically unwell sufferers arrived in a packed ready room on the similar time.
If these sufferers had are available in simply three hours later, he would have been compelled to name a Code Orange — usually reserved for excessive conditions like aircraft crashes — the place each accessible health-care employee locally known as in to attempt to assist hold sufferers alive.
“We might have been scrambling to get as lots of the interventions finished with every of the sufferers that have been concurrently crashing with principally no workers,” he mentioned.
“Fortunately, I believe all of them did effectively ultimately. However once more … had it been within the subsequent shift — who is aware of what would have occurred?”
Sadly, the scenario might be dire for some, with reviews from Quebec, Alberta, Manitoba, British Columbia, New Brunswick and Nova Scotia in the course of the previous 12 months of sufferers tragically dying after ready for hours in crowded hospitals, unable to get the care they want.
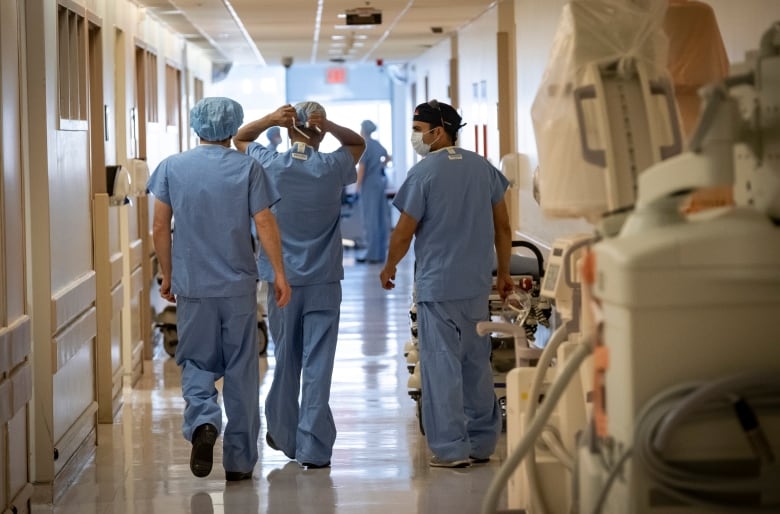
A affected person went into cardiac arrest final week whereas an on-call physician wasn’t on web site at Troopers Memorial Hospital in Middleton, N.S. Paramedics and firefighters tried life-saving measures till the physician arrived, however the affected person didn’t survive.
Well being-care staff are fed up with the scenario, and a whole bunch of emergency physicians in Calgary and British Columbia have signed open letters in current weeks to sound the alarm in regards to the worsening ER disaster.
Final week, 15 nationwide medical organizations representing medical doctors and nurses throughout the nation revealed a joint assertion, calling on the provinces to make reforming the health-care system their high precedence at a gathering of the premiers in Winnipeg subsequent month.
Dr. Urbain Ip, a number one emergency room doctor at Surrey Memorial Hospital, got here ahead final month to talk overtly in regards to the rising disaster in one among B.C.’s busiest ERs and the toll it was taking over workers.
“I reside locally, and I mentioned that is private for me — I can’t confidently ship my family members to my hospital,” he informed CBC Information. “I don’t have to elucidate extra once I’ve labored there for 30 years and I can’t belief that the hospital can handle my household.”
‘Unprecedented challenges’ dealing with health-care system
An ER in Minden, Ont. just lately shut down completely on account of staffing shortages, and the following closest emergency companies are 25 kilometres away, forcing well being officers to announce an pressing care clinic will quickly open on the web site.
Niagara Well being introduced earlier this month that as of July 5, it can completely shut two pressing care centres between 10 a.m. and 10 p.m. so medical doctors might be redeployed to ERs, with a shortfall of 274 doctor shifts between June and August alone.
And a hospital in Prince George, B.C., was compelled to name a Code Orange this week after a close-by deadly bus crash involving 30 individuals pushed workers past capability; town requested anybody with out life-threatening accidents to keep away from visiting the ER.
“Canadians are rightfully involved, and so are we. Nobody ought to lose a cherished one as a result of they couldn’t get well timed medical consideration,” the workplace of federal Well being Minister Jean-Yves Duclos mentioned in a press release to CBC Information.
“The previous couple of years have offered unprecedented challenges for our health-care system. Well being staff, together with people who work in hospitals and emergency rooms, are overwhelmed. Sufferers additionally really feel the pressure after they can’t entry the care they want.”
Knowledge from the Canadian Institute for Well being Data (CIHI) exhibits 90 per cent of sufferers waited over 4 hours in ERs earlier than being seen by a health care provider between March 2021 and April 2022. That’s a bounce from a wait of over three hours between 2017 and 2018.
New figures from Might present sufferers in Ontario emergency rooms are ready longer than ever to be seen by a health care provider. Some are questioning whether or not household medical doctors have to be a part of the answer by seeing extra sufferers in particular person.
For sufferers who have been admitted to hospital, 90 per cent waited virtually 41 hours earlier than getting a mattress within the interval between 2021 and 2022, up from 33 hours in 2017 to 2018.
The longest wait time — over 74 hours — was in Prince Edward Island’s ERs in 2021 to 2022.
A brand new editorial within the Canadian Medical Affiliation Journal is looking for “sensible and fast steps” to be taken to “mitigate harms brought on by lengthy wait-times for emergency care” and “shield the emergency health-care suppliers” shouldering the disaster.
“One of many issues that front-line suppliers are extraordinarily good at doing is creating workarounds, so the impacts of elements of the system which are falling aside usually are not felt by the affected person,” mentioned Dr. Alika Lafontaine, president of the Canadian Medical Affiliation.
“What you’re actually seeing within the final couple of years is an lack of ability of front-line suppliers to do this anymore, both as a result of they themselves really feel such a heavy burden that they bodily, emotionally and mentally simply can’t do it, or that the stresses on the system are too nice.”
Peggy Holton, a nurse at Surrey Memorial Hospital with many years of expertise, mentioned it’s vital for Canadians to grasp that the unsustainable pressures dealing with ERs are affecting sufferers, in addition to health-care staff.
“We’re very resilient as nurses and medical doctors — we’re an excellent crew. However the fixed demand has definitely taken its toll. It’s morally and ethically very demanding on sufferers and on the health-care workers,” she mentioned.
“Typically the demand is simply so excessive that we are able to’t get to all people. And so it’s inflicting lots of psychological and ethical misery … to the purpose the place that’s why persons are leaving.”

A part of the issue, Holton mentioned, is nurses aren’t delivered to the desk to debate options, however they’re on the entrance traces of the disaster and sometimes the primary place the place anger and abuse is directed in a dysfunctional system.
“We have to have stronger insurance policies in place that may assist the nurses with violence within the office. We additionally want to sit down collectively and have a look at how can we recruit workers, how can we retain workers?” she mentioned.
“One nurse informed me the opposite day that ‘there isn’t a day that I’m going to work that I’m not both verbally, bodily or sexually assaulted by both a affected person or a member of the family.’ And that’s actually unhappy.”
‘Operating on hope’
Ip’s choice to come back ahead earlier this month, alongside dozens of colleagues, in regards to the dire scenario at Surrey Memorial led the B.C. authorities to take fast motion to rent extra workers and handle rising shortfalls in funding and broaden companies in key areas.
“We’re working on hope proper now,” mentioned Ip, including he and his colleagues started taking over extra shifts once more after the announcement. “This raises morale, and when morale is sweet, individuals will step as much as the plate. And regardless of how brief we’re, we’re going to make it.”
However hospitals shouldn’t need to be pushed to the brink for modifications to be made to deal with the disaster, he mentioned. And whereas there’s no straightforward reply to the long-standing drawback, there are tangible areas that want addressing to assist ease the issues plaguing ERs.
A key a part of the issue is funding, however there are deeper points that have to be addressed past the hospital, front-line health-care staff mentioned, together with an absence of entry to household medical doctors, in addition to beds in long-term care and residential care that pressure sufferers to show to the ER.
Canada is dealing with a important scarcity of household medical doctors, with thousands and thousands of Canadians with out entry to major care due to retiring physicians and fewer medical college grads selecting the specialty on account of an absence of sources and excessive overhead prices.
Virtually half of adults throughout Canada’s 10 provinces had issue accessing well being care in 2020 and 2021, whereas shut to fifteen per cent mentioned they didn’t obtain all of the care they wanted, in line with a 2021 survey from Statistics Canada.
Some communities in Ontario are turning into ‘physician deserts’ on account of a spike in retirements of household physicians and never sufficient younger physicians to switch them. The CBC’s Mike Crawley zeros in on the disaster in a province the place 1.8 million individuals don’t have a household physician.
“Even in the event you mentioned, we’re going to graduate double the variety of physicians now, it’s at the least 5 to 10 years away earlier than we might have sufficient physicians,” mentioned Sehgal, in Fredericton.
“Within the interim, and even long run, you’re going to want individuals like doctor assistants, nurse practitioners, nurses, pharmacists … [and] medics working past what they’re doing proper now.”
Dr. Marc Beique, an ER doctor on the McGill College Well being Centre, mentioned there isn’t a straightforward reply to the worsening issues dealing with ERs, however there must be a complete rethink of how care is supplied, how sufferers are supported and the place they select to entry care.
“We’re not in a dynamic the place you may clear up 80 per cent of the issues with one answer. The fact is that you just’re gonna have to resolve 10 per cent right here, 10 per cent there and 10 per cent there — and it must be a concerted, clever and considerate endeavour,” he mentioned.
“I strongly consider that we are able to get there, I believe it’s potential. And personally, I consider within the public system and I believe that’s the best way to go.”
Lafontaine mentioned the truth that provincial and territorial governments haven’t been required to spend funding that they obtain from the federal authorities for well being care instantly on the system for the previous a number of many years is worsening the issue.
A scathing report from the Monetary Accountability Workplace of Ontario earlier this 12 months discovered hospital capability will proceed to fall by 2027-2028 on account of elevated demand for companies, an ageing inhabitants and the underfunding of the well being sector by $21.3 billion.

“The ER is the final line of defence. Primarily as a result of the ER, in the entire health-care system, is the one place the place you may’t say no,” mentioned Beique. “So lots of sufferers will find yourself within the emergency for non-emergency causes, however principally as a result of they’ve nowhere else to go.”
The scenario has turn out to be so difficult that just about one in 5 sufferers displaying as much as the College of Montreal Well being Centre’s emergency division depart earlier than ever being seen by a health care provider, in line with a brand new report obtained by the Montreal Gazette.
“If nothing occurs that’s totally different than what we’re doing right this moment, the whole system will burn down till there’s nothing left. And I do know that that’s a really heavy factor to say. However that’s the actuality,” mentioned Lafontaine.
“We both intervene, or we do nothing, and issues will degrade to the purpose that we’ll not have a health-care system on this nation.”

